The Age at Which a Baby Was Weaned Quizlet
- Review
- Open Access
- Published:
Baby-led weaning: what a systematic review of the literature adds on
Italian Periodical of Pediatrics book 44, Article number:49 (2018) Cite this article
Abstruse
The term weaning describes the fourth dimension period in which a progressive reduction of breastfeeding or the feeding of infant-formula takes place while the infant is gradually introduced to solid foods. It is a crucial time in an infant's life equally not but does information technology involve with a great deal of rapid modify for the kid, only it is also associated with the development of food preferences, eating behaviours and body weight in childhood and also in adolescence and machismo.
Therefore, how a kid is weaned may accept an influence afterward, on the individual'due south entire life. Babies are traditionally first introduced to solid foods using spoon-feeding, in most countries.
Beside to traditional approach, an alternative method, promoting infant self-feeding from 6 months of age, chosen baby-led weaning or "auto-weaning", has grown in popularity. This approach causes concern to healthy professionals and parents themselves as information from observational studies pointed out to a potential gamble of iron and energy inadequacy as well as choking risk. Aim of this systematic review was to critically examine the current evidence virtually infant-led weaning approach and to explore the need for future research.
A systematic search was conducted in Cochrane library databases and Cartel (Database of Abstract of Reviews of Furnishings), EMBASE and MEDLINE in the flow 2000–2018 (upwardly to March 1st) to address some key questions on baby-led weaning. Prisma guidelines for systematic reviews has been followed.
After the inclusion/exclusion process, we included for analysis of evidence 12 articles, x observational cross-sectional studies and 2 randomized controlled trials. Pooling of results from very dissimilar outcomes in the studies included was not possible. Both randomized trials have potential bias; therefore, the quality of the evidence is low.
There are still major unresolved issues nigh baby-led weaning that require answers from research and that should be considered when advices are requested from health professionals by parents willing to arroyo this method.
Background
The term weaning describes the time period in which a progressive reduction of chest-feeding or the feeding of infant-formula takes place while the babe is gradually introduced to complementary foods. The introduction of complementary foods during the weaning period is by and large progressive, and leads the infant to accomplish the dietary blueprint of an adult within the 2d year of life [1].
The Earth Health Organisation (WHO) recommends exclusive breastfeeding for the first six months of historic period, and complementary breastfeeding at least until the 2nd twelvemonth of age. According to the WHO, the introduction of complementary foods should exist safe, well-timed and acceptable; information technology should start when exclusive breastfeeding tin no longer provide enough nutrients and free energy for the infant'due south growth and evolution, and it should contain foods that offer these nutrients and free energy [ii]. The weaning period is a crucial time in an baby'due south life since it not only involves a smashing deal of rapid change for the child, but it is also associated with the development of food preferences, eating behaviours and torso weight in childhood, adolescence too every bit in machismo.
Babies are traditionally first introduced to solid foods using spoon-feeding of specially prepared sparse purées. Later on, following the babe's historic period and developmental progress, the foods offered gradually shift towards family unit foods [iii].
Over the terminal 10–xv years, an alternative approach known every bit "babe-led weaning" (BLW), or "car-weaning", has grown in popularity, particularly in the United Kingdom and New Zealand and more recently besides in other countries in Europe [4, 5]. The term "infant-led" weaning was first coined by Gill Rapley in 2005 [6]. BLW is an alternative method of infant feeding which promotes infant self-feeding from six months of historic period, instead of conventional parent spoon-feeding. Although BLW is not particularly mentioned in the WHO'southward recommendations, it is becoming more than pop. The key features of BLW are that infants participate in family unit mealtimes, and 'whole' (babe-fist size) pieces of food are offered to them, and so they feed themselves from the beginning of complementary feeding, at around 6 months of age [7]. Information technology means that although parents offering foods, the child himself controls the weaning process (thus the term "baby-led"): infants decide what, how much and how apace to consume [8]. The term underlines the fact that the infant is an active partner in the feeding process, and not a passive recipient to fill with food [9].
BLW may too exist defined equally motorcar-weaning, which ways offering chopped and minced family meals to the infants [10]. While in the traditional weaning infants are offered puréed babe foods that are frequently fabricated upwardly of several ingredients, in the baby-led weaning a variety of single picked foods is offered to the baby. In the one-time approach, the tastes of the single foods are mixed together and the child is not always able to distinguish them; conversely, BLW approach might provide an early and more stable learning almost the satiating capacities of foods and therefore it may enable a better satiety-responsiveness [11].
BLW seems to be associated with other positive aspects, such as lower maternal feet and command during the weaning menstruum, only this point is controversial [12].
A recent review has found that many mothers utilize food to influence infant growth, contentment and sleep and that they choose ease of feeding over babe feeding recommendations [thirteen].
However, this approach as well causes concerns in chief care paediatricians and in parents themselves, regarding main topics such equally atomic number 26 adequacy [14, xv], energy and nutrient intake and choking risk [10].
The European Society for Paediatric Gastroenterology, Hepatology and Diet (ESPGHAN 2017), in a recent position paper, stated that there is not enough evidence to draw conclusions near the BLW approach [xvi]. At the same fourth dimension, a not-systematic review past Dark-brown et al., because the available literature on BLW upward to December 2016, came to like conclusions [four].
Aim
The aim of this systematic review was to critically examine the current evidence about the BLW approach, in order to assess whether it is safe and advisable for parents and infants too as to explore the demand for hereafter research.
Methods
We aimed to address the following Fundamental Questions:
- 1.
Does BLW increase risk of choking?
- 2.
Does BLW make up one's mind adequate energy intake and normal growth?
- 3.
Does BLW crusade an increased adventure of inadequate iron intake and resulting suboptimal atomic number 26 condition?
- 4.
Which furnishings has the BLW approach on satiety-responsiveness and weight?
- 5.
Does BLW influence food preferences and nutrition quality?
- 6.
Does BLW improve family unit relationships during shared meals?
- seven.
Practise mothers who adopt a infant-led arroyo differ from those who cull traditional weaning regarding the starting fourth dimension of complementary feeding?
- 8.
Does BLW take positive effects on mother anxiety and attitude towards complementary feeding?
To reply these Key Questions nosotros searched, from 2000 up to March 1, 2018 the Cochrane Database of Systematic Reviews and DARE (Database of Abstract of Reviews of Effects), for terms "weaning" and "baby-led weaning".
The details of search strategies in PubMed (MedLine) and EMBASE are listed in Table 1.
Nosotros planned hand-search for other relevant articles from selected papers.
Our inclusion criteria, with respect to the predefined aims of the review, were: evidence-based guidelines, systematic reviews, randomized controlled trials, controlled clinical trials and observational studies that compared outcomes related to growth and development, energy, macro- and micronutrient intake and feeding attitudes in children and families that are following BLW approach or standard/traditional complementary feeding; outcomes related to the touch on of unlike weaning styles on mothers feelings and attitudes about their children are considered.
No exclusions were made for age nor restriction for language.
Practice guidelines not show-based, narrative reviews, editorials, other publication types and manufactures in which BLW was not clearly defined and/or quantified, were considered for discussion of items but excluded from formal analysis and from tables of evidence.
We planned to appraise the relevant guidelines with the AGREE Two instrument [17], systematic reviews with the AMSTAR-2 tool (A MeaSurement Tool to Appraise systematic Reviews) [eighteen], Randomized Controlled Trials with the Assessment of Chance of Bias Cochrane tool [19], Observational studies with the Newcastle-Ottawa Scale, modified for cross-sectional studies [xx].
ED and MB independently searched and selected the literature based on the inclusion/exclusion criteria, then extracted results and appraised the included articles.
We considered methodological lacks of each written report to answer Fundamental Questions.
We likewise planned the pooling of results, with appropriate methods, if the same outcome was nowadays in a sufficient number of not heterogeneous studies.
Results
After the inclusion/exclusion process, we included 12 articles, ten observational cantankerous-sectional studies and 2RCT (from the same population) for analysis of testify.
In Fig. 1 nosotros show the PRISMA Catamenia Diagram [21] of search and selection.
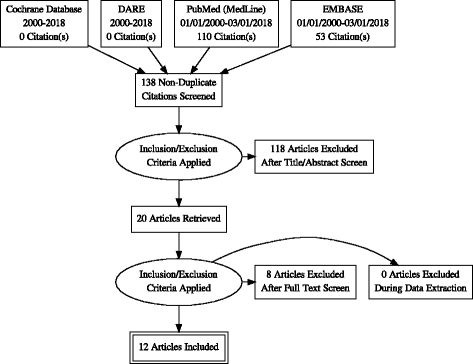
PRISMA Flow Diagram
The characteristics of the included studies are listed in Table 2 and described in the text answers to Primal Questions.
Trials excluded from formal assay subsequently full-text screening are listed in Appendix 1, with motivations for exclusion.
Pooling of results from very different outcomes in the studies included was not possible.
- Does BLW increase run a risk of choking?
Choking tin easily occur in infants learning to eat, because they are moving foods around the mouth, chewing and biting for the first times; at six months, the baby may have not yet developed the oral motor skills required to safely ingest whole foods (such as chewing and swallowing) [10, 22].
There may exist a discrepancy betwixt the babe's apparent power to cocky-feed and the real capacity to do then; not all 6-month- old children are developmentally ready to kickoff feeding solids [23].
A small survey constitute no differences in choking incidence betwixt BLW and traditional weaning groups [24]. In 199 BLW infants, xxx% had at to the lowest degree one episode of choking with solid food ingestion (apple). It cannot be excluded that this loftier rate was caused by parents' difficulties to distinguish choking from gagging [25].
Similar results were establish past Brown et al. in a recent observational report on 1151 infants addressing the hazard of choking and gagging. The results of the study showed at least 1 episode of choking had occurred in 11.nine% of the strict BLW group, in xv,5% of the loose BLW grouping and in eleven.6% of the traditional weaning group, without significant differences among groups [26].
It should exist noted that this study is not a randomized study, and that it considers a self-selected sample of mothers, that could lead to less reliable results.
Likewise, a randomized study by Fangupo et al., specifically designed to accost the risk of choking, found no differences in choking episodes between the unlike weaned groups [27].
Fangupo et al., all the same, did not consider a classical BLW sample of children, but a modified version of BLW, the BLISS [(Babe-led Introduction to Solids (BLISS)] method, providing written and verbal letters to allow parents to larn how to avoid foods more related to choking chance, such every bit raw apple and grapes, even associated to fatal choking [24, 28, 29]. Hence, it is possible that unmodified BLW may not have the same effects.
The BLISS method was developed and tested by Cameron et coll in 2015 [29].
They aimed to specifically accost the concerns of healthcare professionals towards an inadequacy of atomic number 26 and energy intake, besides equally the take chances of choking when post-obit BLW. The BLISS method consists of several essential characteristics including offering foods and so that the infant tin feed themselves like to a BLW approach, but additionally the method includes communication to offer one high-atomic number 26 food at each meal, i loftier-energy food at each repast and nutrient being prepared suitably according to the infant'due south level of development to reduce the chance of choking, every bit well as avoiding loftier choking-risk foods [27, 29]. The difference between BLW and Bliss is mainly the level of specificity of the instructions, while the key characteristics remain the same.
The pilot written report by Cameron has some important limitations, such as a missing group of traditional weaned infants, no random consignment to the groups and only recruiting parents who already planned to employ a baby-led approach earlier-mitt. This means that parents who felt confident well-nigh the BLW method would rather assign to the BLW group, while parents who felt they needed extra support would choose to assign to the Bliss grouping. Despite its limitations, this study firstly introduced a modified version of BLW, in which detailed and written instruction are given to the parents.
- Does BLW determine increased chance of inadequate energy intake and growth faltering?
The results from the observational study by Townsend et al. reported that more BLW children were classified as significantly underweight, compared to spoon-fed children [24]. Another observational study underlined that mothers following a BLW approach estimated that their babies ate more than milk feeds and less solid food compared to those post-obit a traditional weaning; this may provide inadequate nutrient intake for infants from six months of age onwards [30]. Recently, Morison et al. reported that even though total energy intake was like between a BLW and a traditional spoon-fed group of infants, BLW infants appeared to consume more total fatty and saturated fat than traditional spoon-fed [31].
In agreement with the observational report by Morison et al., the randomized report by Taylor showed no differences in energy intake between the Bliss group and the control group [32].
Additionally, none of the baby-led children in the sample showed growth faltering.
The discrepancies in results compared to the previous studies may be due to the unlike written report design, or to the fact that those studies used babe weight reported by parents, whereas Taylor et colleagues direct measured the infants' weight. It is also important to address the fact that the BLISS study participants were encouraged to include a loftier-energy food at each meal, which may accept attenuated the run a risk of growth faltering.
- Does BLW cause inadequate iron intake and suboptimal iron condition?
From six months onwards, breastfeeding does not provide the infant with enough iron to satisfy requirements; therefore, an increased corporeality of iron is needed from complementary foods. To address this purpose, atomic number 26-fortified infant cereals and commercial meat-based infant foods are by and large offered. BLW infants may exist at risk of inadequate iron intake as the consistence of these foods makes them difficult for babies to cocky-feed. Furthermore, nearly easily graspable foods, such as fruits and vapour cooked vegetables, which are the most commonly introduced during BLW, are known to be mostly depression in iron [25, 33].
Upwardly to now, this issue has been formally addressed in the Bliss study by Cameron et al. [29].
Subjects in the Bliss grouping were offered more than portions of fe rich foods at half dozen months and had a college introduction of iron containing foods in the beginning weeks of introduction of solid foods compared to those in BLW group.
Although there was no statistically significant departure in the amount of iron intake from complementary foods by the Elation and BLW participants who completed the diet records, it must be considered that the sample size was very pocket-size (four in each group). Noteworthy, none of the eight infants for whom diet record data were available were able to achieve the WHO recommendation for iron intake from complementary foods.
- Which effects has the BLW approach on satiety-responsiveness and weight?
To date, three studies aimed to evaluate the influence of chosen eating feeding on salubrious-related outcome, such equally trunk mass alphabetize (BMI) and obesity [eleven, 24, 34]. Townsend and Pitchford institute a higher occurrence of underweight children in the infant-led group (three/63) and an increased incidence of obesity in the spoon-fed group (8/63); however, it should exist pointed out that 32% of the data on BMI was missing in the baby-led grouping [24].
In another larger, cross-sectional written report Chocolate-brown and Lee institute no association between the weaning approach (BLW vs spoon feeding) and parentally reported infant weight at six months of age [34].
A subgroup of participants in this study were and so evaluated at eighteen–24 months; the aim of this self-reported observational, comparative study was to examine the effect of different weaning practice on child satiety-responsiveness and weight at 18–24 months [xi]. Children who were introduced to solids on a BLW approach were reported to be significantly less nutrient responsive, less fussy and more than satiety-responsive compared to the traditional weaning group. The authors found that toddlers who had followed BLW had lower mean body weight than the spoon-feeding approach. Again, these findings need to exist treated with caution, considering the weight was self-reported and the overall number of children in an overweight-range was small-scale in this report. Furthermore, a lot of differences have been shown amongst parents who followed BLW and traditional weaning, which can influence weight.
The same outcomes were evaluated in a recent randomized clinical trial by Taylor and colleagues [32]. Differently from the previous studies, they found no significant differences in BMI at 12 and 24 months between the baby-led group and the traditionally fed 1. In contrast with Brown and Lee, baby-led infants resulted to be less satiety responsive at 24 months of historic period. Besides the study past Taylor, nonetheless, did not consider a classical BLW sample of children, but a Elation one. It is possible that unmodified BLW may not accept the same effects every bit this case.
- Does BLW influence food preferences and nutrition quality?
Information technology has been hypothesized that BLW may promote acceptance of a wider range of food equally a issue of different tastes and textures from the variety of offered foods [33]. This attribute has been formally addressed in ii observational studies.Morison BJ et al. found no differences in food preferences between BLW and traditional weaned infants [31]. Conversely, Townsend et al. observed that BLW weaned children had a preference for carbohydrates, whereas the spoon-fed infants preferred sweets [24]. These results require circumspection as this observational study was based on a retrospective recall of a weaning approach.
Another relevant upshot regards the quality of the meals consumed by BLW infants.
Commercial baby foods or abode-prepared purées practice non usually include sugar and salt. On the other hand, family foods may not always be suitable for infants, specifically regarding the way of cooking and dressing. For instance, if the family ordinarily swallow candy foods or salty foods (i.due east, foods flavoured with salt, stock cubes or salad dressing) or snacks, sweets and cereal bars, that infant is likely to be offered it too.
With regard to this issue, the Elation Study showed that Bliss group consumed college levels of sodium [35].
Concerns have been expressed that, eating foods which are inappropriate for infants, BLW babies might get accepted to carbohydrate and salt tastes [22], potentially resulting in increased consumption, which may in turn influence some wellness outcomes (e.g blood pressure level) already during childhood [36].
To avoid these risks, parents should receive a proper nutritional educational activity to brand their diet healthy and adequate for the infant.
Further studies are needed to specifically address the impact of infant-led weaning on food preferences and choices during childhood and later health outcomes.
- Does the baby-led approach improve family relationships during shared meals?
It has been proposed that BLW children may participate in mealtimes more than easily than traditional spoon-fed children, because they consume the aforementioned foods with the residuum of the family. At the aforementioned time, as BLW infants are never forced to consume food, there may be less mealtime pressure and anxiety. Withal, a unmarried non-comparative cantankerous-sectional study found that BLW does non amend the family's eating style [37].
- Practise mothers who adopt a baby-led approach differ from those who choose traditional weaning regarding the starting time of complementary feeding?
Information technology is non articulate if BLW leads to starting complementary feeding subsequently, or if parents who manage to expect until the sixth calendar month of age adopt a BLW approach.
According to the information from observational studies, mothers choosing to follow a baby-led approach appear more probable to begin complementary feeding at six months of age [26, xxx, 38]. Data derived from randomized trial are lacking.
As there is some evidence that introduction to solids before six months may increase the run a risk of overweight in childhood [39], further research is warranted to accost this issue.
- Does BLW have positive effects on mother anxiety and attitude towards complementary feeding?
Babe-led mothers reported lower anxiety, lower obsessive-compulsive disorder scores, lower eating restraints and higher conscientiousness than traditional weaning mothers every bit shown by the observational report by Dark-brown et al. [40]. These maternal characteristics might make a BLW approach more feasible; however, this finding may also be explained by a reverse causality, according to the fact that mothers high in anxiety may exist more probable to cull a traditional weaning approach, where there is more than existing literature and support from healthcare professionals, and where the infant's intake is strictly controlled via spoon-feeding.
Give-and-take
One of the critical aspects of the BLW approach is that no formal definition exists. In its purest form, BLW should not include any spoon-feeding and the child himself should put foods into his mouth. Equally a limitation, nearly existing studies on the baby-led approach include participant families who self-place as following a BLW. In some studies, participants were asked to gauge the utilise of spoon-feeding opposed to self-feeding and the amount of puréed foods given during the weaning menstruation in per centum [11, 12, 30, 34]. In others, they were just asked to identify themselves every bit followers of BLW approach [14, 24, 31]. It is unclear whether BLW can include limited use (less than 10%) of purées and spoon-feeding, or if it is ruled by a more than strict definition, where exclusively finger foods are provided. Really, both views exist amongst parents who believe in a baby-led style infant feeding [33]. Concerning the method of recruitment, most studies recruited via internet sites, that tin can represent a selection bias [41]. A recent research conducted in the UK institute that mothers following a baby-led approach were more likely to have higher levels of pedagogy, and a professional occupation, compared to mothers choosing traditional weaning. This may exist due to the fact that the population group with higher education is more likely to accept increased cyberspace access, which is likewise one of the main information sources about BLW [25, 30].
Overall, the bear witness nigh BLW is by and large derived from observational studies, of which only comparative cantankerous-sectional studies were formally analyzed. The methodological quality of the included studies is generally very low, except for two studies, (Table 3).
Therefore, the observed results need to exist treated with caution. Every bit regards the major concerns about the BLW approach, e.k. inadequate energy intake and choking risk, there are very few information on the role of the paediatrician's support on this practice. Although the randomized studies by Taylor and Fangupo specifically addressed these issues, in the aforementioned cohort, both of them have methodological weaknesses that telephone call into questions the results (Table four).
Most of the outcomes were cocky-reported, the intention to treat analysis was not performed and both had a high rate of drop-out. Moreover, the evaluation of nutrient intakes has not been included in the secondary outcomes of the study, but has been described just in an unpublished doctoral dissertation by Erickson, that examines initial findings of the BLISS Written report, considering adherence to the weaning approach and nutrient intake, respectively [35]. Therefore, this issue needs a careful monitoring by the paediatrician in order to ensure adequate growth.
Even with the higher up mentioned limitations, the Bliss Study suggests that this kind of approach, employing resources and methods to educate participants, may be suitable to be tested in further randomized controlled trials.
Anyway, parents willing to follow BLW approach demand a conscientious and deeper nutritional education in order to avoid whatsoever hazard to their infants. In particular, they should be given advice on how to ready foods in such a fashion they effect safe, healthy and nutritious.
The office of different approaches to weaning in the evolution of the early-life gut microbiome is an additional interesting attribute, which has not however been investigated. Information technology is known that changes in the nutrition limerick can alter the prevalence and types of microbial species living in the gut, as certain species are improve equipped to use specific substrates [42].
The showtime solid foods introduced could therefore play a fundamental role in shaping the infant's gut microbiome. A recent study, assessing the effect of fe supplementation in infants, constitute that children fed iron-only fortified cereals, or puréed meats, iron- and zinc-fortified cereals, equally the primary complementary foods until 9–10 months of age, had different prevalence in the gut microbial species [43]. The former had a relative decrease with time in the genera Bifidobacterium and Rothia and in the social club Lactobacillales, and an abundance of the order Bacteroidales, compared to the latter. Further investigations are needed to determine if the BLW arroyo could shape the microbiome in a dissimilar way compared to the traditional weaning.
Another relevant issue is that in the BLW approach children are exposed to a wide range of family foods in a relatively early and mixed manner and sometimes also to packaged foods, which can incorporate multiple food allergens. Therefore, in example of reaction, it can be difficult to identify the specific food allergen involved.
This potential risk has not been formally investigated, fifty-fifty though the weaning period requires special attending, particularly in children at loftier gamble of allergy.
Conclusions
Currently, there is still bereft show to draw conclusions well-nigh the BLW arroyo, in terms of adequacy of energy and nutrient intakes, due to the low quality of the bear witness. In fact, concerns persist since some previous observational studies indicated that mothers using the BLW approach estimated that their babies ate more milk feeds and less solid foods compared to those post-obit a traditional weaning, focussing attention on inadequate nutrient intakes for infants from half dozen months of age onwards. Nonetheless, other testify from more contempo randomized studies propose that a modified BLW approach (BLISS Written report), including recommendations about the introduction of selected iron-rich foods, besides every bit fugitive foods at gamble of choking, might have positive preventive effects on the risk of choking and nutrients deficiency. Thus, these issues require further investigation in larger randomized studies.
In summary, at that place are even so major unresolved issues in BLW that require answers from enquiry, which should exist considered when advices are requested from health professionals by parents willing to follow the BLW approach (Table five).
References
-
EFSA Panel on Dietetic Products. Diet and allergies (NDA). Scientific opinion on the appropriate historic period for introduction of complementary feeding of infants. EFSA J. 2009;vii:1423.
-
World Health Arrangement. UNICEF. Global strategy on baby and immature child feeding. Geneva: Earth Health Arrangement; 2002. http://world wide web.who.int/nutrition/publications/infantfeeding/9241562218/en/
-
Earth Wellness Organization. Infant and Young Kid Feeding. Model chapter for textbooks for medical students and allied health professionals. Geneva: World Health Arrangement; 2009.
-
Brown A, Jones SW, Rowan H. Baby-led weaning: the evidence to date. Curr Nutr Rep. 2017;6:148.
-
Caroli M, Mele RM, Tomaselli MA, Cammisa M, Longo F, Attolini E. Complementary feeding patterns in Europe with a special focus on Italy. Nutr Metab Cardiovasc Dis. 2012;22:813–eight.
-
Rapley G. Infant-led weaning. In: Maternal and Infant Nutrition and Nurture: Controversies and Challenges (5 Hall Moran, F Dykes eds). London: Quay Books. 2005;275–98.
-
Rapley G, Murkett T. Baby-led weaning: helping your baby dearest expert food. London: Vermilion; 2008.
-
Rapley G. Baby-led weaning: transitioning to solid foods at the babe's ain stride. Community Pract. 2011;84:20–iii.
-
Sachs M. Baby-led weaning and electric current UK recommendations - are they compatible? Matern Child Nutr. 2011;7:one–2.
-
Alvisi P, Brusa Due south, Alboresi South, Amarri S, Bottau P, Cavagni G, et al. Recommendations on complementary feeding for good for you, full-term infants. Ital J Pediatr. 2015;41:36.
-
Brown A, Lee MD. Early on influences on child satiety-responsiveness: the role of weaning style. Pediatr Obes. 2015;10:57–66.
-
Dark-brown A, Lee M. An exploration of experiences of mothers following a baby-led weaning style: developmental readiness for complementary foods. Matern Kid Nutr. 2013;9:233–43.
-
Harrison G, Brodribb Westward, Hepworth J. A qualitative systematic review of maternal infant feeding practices in transitioning from milk feeds to family foods. Matern Child Nutr.2017;xiii:e12360. https://doi.org/10.1111/mcn.12360.
-
Cameron SL, A-LM H, Taylor RW. Healthcare professionals' and mothers' knowledge of, attitudes to and experiences with, baby-led weaning: a content assay study. BMJ Open. 2012;2:e001542.
-
Carter RC, Jacobson JL, Brunt MJ, Armony-Sivan R, Dodge NC, Angelilli ML, et al. Iron deficiency anemia and cognitive function in infancy. Pediatrics. 2010;126:e427–34.
-
Fewtrell K, Bronsky J, Campoy C, Domellöf K, Embleton Due north, MisN F, et al. Complementary feeding: a position paper past the European Order for Paediatric Gastroenterology, hepatology, and nutrition (ESPGHAN) committee on diet. J Pediatr Gastroenterol Nutr. 2017;64:119–32.
-
Brouwers M, Kho ME, Browman GP, Cluzeau F, Feder Chiliad, Fervers B, et al. Agree next steps consortium. Concord 2: advancing guideline development, reporting and evaluation in healthcare. CMAJ. 2010;182:E839–42.
-
Shea BJ, Reeves BC, Wells Thou, Thuku M, Hamel C, Moran J, et al. AMSTAR two: a disquisitional appraisal tool for systematic reviews that include randomised or not-randomised studies of healthcare interventions, or both. BMJ. 2017;j4008:358.
-
Higgins JPT, Greenish S, editors. Cochrane handbook for systematic reviews of interventions [updated march 2011]. Chichester: Wiley-Blackwell; 2011.
-
Wells GA SB, O'Connell D, Peterson J, Welch Five, Losos M, Tugwell P. The Newcastle-Ottawa scale (NOS) for assessing the quality of nonrandomized studies in meta-analyses.http://www.ohri.ca/programs/clinical_epidemiology/oxford.htm. Accessed one November 2017.
-
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Grouping (2009). Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ. 2009;339:b2535.
-
Daniels 50, Heath AL, Williams SM, Cameron SL, Fleming EA, Taylor BJ, et al. Baby-led introduction to SolidS (Bliss) study: a randomised controlled trial of a infant-led approach to complementary feeding. BMC Pediatr. 2015;15:179.
-
Wright CM, Cameron Thou, Tsiaka M, Parkinson KN. Is baby-led weaning feasible? When do babies first reach out for and eat finger foods? Matern Child Nutr. 2011;7:27–33.
-
Townsend E, Pitchford NJ. Babe knows best? The bear on of weaning mode on food preferences and body mass index in early childhood in a instance-controlled sample. BMJ Open. 2012;2:e000298.
-
Cameron SL, Taylor RW, Heath AL. Parent-led or infant-led? Associations betwixt complementary feeding practices and wellness-related behaviours in a survey of New Zealand families. BMJ Open. 2013;three:e003946.
-
Chocolate-brown A. No difference in self-reported frequency of choking betwixt infants introduced to solid foods using a babe-led weaning or traditional spoon-feeding arroyo. J Hum Nutr Diet. 2017. https://doi.org/10.1111/jhn.12528.
-
Fangupo LJ, Heath ALM, Williams SM, Erickson Williams LW, Morison BJ, Fleming EA, Taylor BJ, Wheeler BJ, Taylor RW. A Baby-Led Approach to Eating Solids and Chance of Choking. Pediatrics. 2016;138(iv):e20160772. https://doi.org/ten.1542/peds.2016-0772.
-
Hayman RM, Dalziel SR, Baker NJ, Kid and Youth Mortality Review Committee. Special report: unintentional suffocation, foreign trunk inhalation and strangulation. Wellington: Kid and Youth Bloodshed Review Committee; 2013.
-
Cameron SL, Taylor RW, Heath AL. Evolution and pilot testing of baby-led introduction to SolidS--a version of baby-led weaning modified to address concerns nigh iron deficiency, growth faltering and choking. BMC Pediatr. 2015;15:99.
-
Brown A, Lee MA. Descriptive study investigating the use and nature of babe-led weaning in a United kingdom of great britain and northern ireland sample of mothers. Matern Child Nutr. 2011;7:34–47.
-
Morison BJ, Taylor RW, Haszard JJ, Schramm CJ, Williams Erickson 50. FangupoLJ, et al. how different are infant-led weaning and conventional complementary feeding? A cross-sectional written report of infants aged 6-8 months. BMJ Open. 2016;vi:e010665.
-
Taylor RW, Williams SM, Fangupo LJ, Wheeler BJ, Taylor BJ, Daniels 50, et al. Effect of a baby-led approach to complementary feeding on InfantGrowth and overweight: a randomized clinical trial. JAMA Pediatr. 2017;171:838–46.
-
Cameron SL, Heath AL, Taylor RW. How feasible is baby-led weaning as an approach to infant feeding? A review of the bear witness. Nutrients. 2012;4:1575–609.
-
Brownish A, Lee M. Maternal control of child feeding during the weaning period: differences between mothers following a baby-led or standard weaning approach. Matern Kid Health J. 2011;15:1265–71.
-
Erickson LW. A Baby-Led arroyo to complementary feeding: Adherence and baby nutrient and nutrient intakes at seven months of historic period. Doctoral dissertation. University of Otago, 2015. http://hdl.handle.cyberspace/10523/6041
-
Shi L, Krupp D, Remer T. Salt, fruit and vegetable consumption and blood pressure development: a longitudinal investigation in good for you children. Br J Nutr. 2014;111:662–71.
-
Rowan H, Harris C. Baby-led weaning and the family nutrition. A pilot study. Appetite. 2012;58:1046–ix.
-
Moore AP, Milligan P, Goff LM. An online survey of knowledge of the weaning guidelines, communication from health visitors and other factors that influence weaning timing in UK mothers. Matern Child Nutr. 2014;10:410–21.
-
Moorcroft KE, Marshall JL, McCormick FM. Association between timing of introducing solid foods and obesity in infancy and childhood: a systematic review. Matern Child Nutr. 2011;7:three–26.
-
Brown A. Differences in eating behaviour, well-being and personality betwixt mothers post-obit baby-led vs. traditional weaning styles. Matern Child Nutr. 2016;12:826–37.
-
Gosling SD, Vazire Southward, Srivastava S, John OP. Should we trust web-based studies? A comparative analysis of six preconceptions about internet questionnaires. Am Psychol. 2004;59:93–104.
-
Arrieta MC, Stiemsma LT, Amenyogbe N, Brown EM, Finlay B. The intestinal microbiome in early on life: health and disease. Front Immunol. 2014;5:427.
-
Krebs NF, Sherlock LG, Westcott J, Culbertson D, Hambidge KM, Feazel LM, et al. Effects of different complementary feeding regimens on iron condition and enteric microbiota in breastfed infants. J Pediatr. 2013;163:416–23.
Availability of data and materials
Please contact authors for data requests.
Writer information
Affiliations
Consortia
on behalf of the Italian Order of Pediatrics
Contributions
ED: co-conceived and drafted the manuscript; searched and selected literature and critically analyzed the studies. MB: searched and selected literature and critically analyzed the studies. AMS: participated in the pattern of the study and coordination. GB: helped draft the manuscript. EP: helped analyze the selected studies. FP: helped draft the manuscript. GVZ: critically revised the manuscript. DGP: conceived the study and participated in its coordination. All authors have read and approved the final manuscript.
Respective author
Ethics declarations
Ethics approval and consent to participate
Not applicative.
Competing interests
The authors declare that they have no competing interests
Publisher'southward Notation
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix
Appendix
Rights and permissions
Open Access This commodity is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Eatables license, and signal if changes were made. The Creative Eatables Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zilch/1.0/) applies to the data made available in this article, unless otherwise stated.
Reprints and Permissions
Near this commodity
Cite this commodity
D'Auria, E., Bergamini, M., Staiano, A. et al. Baby-led weaning: what a systematic review of the literature adds on. Ital J Pediatr 44, 49 (2018). https://doi.org/10.1186/s13052-018-0487-viii
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/10.1186/s13052-018-0487-8
Keywords
- Choking Risk
- Weaning Arroyo
- Traditional Weaning
- Inadequate Atomic number 26 Intake
- Complementary Foods
Source: https://ijponline.biomedcentral.com/articles/10.1186/s13052-018-0487-8
0 Response to "The Age at Which a Baby Was Weaned Quizlet"
Post a Comment